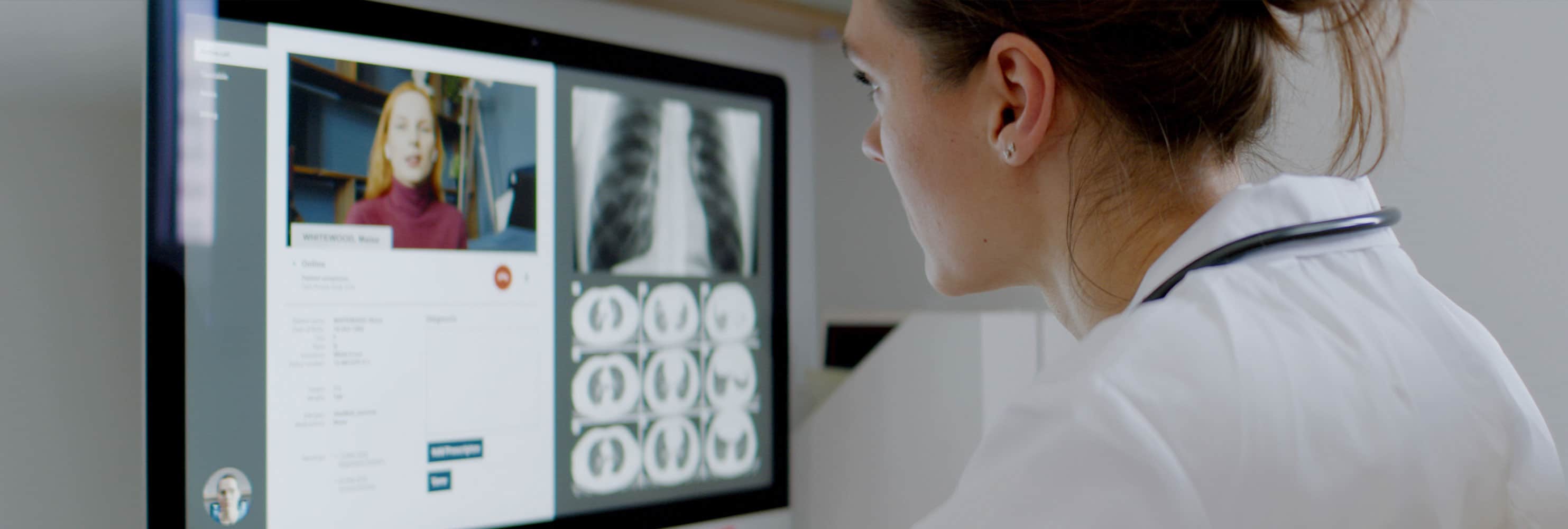
Why Practices Should Still Utilize Telehealth Amid COVID-19
COVID-19 prompted a widespread adoption of telehealth solutions across the country. Pro...
April 13, 2020
The Centers for Medicare and Medicaid Services (CMS) has taken action to prepare the US healthcare system for the surge in patients, related to the coronavirus pandemic. At the beginning of March, Congress lifted barriers to telehealth care, such as geographical restrictions, to simplify access through the duration of the coronavirus. This bill titled the “Coronavirus Preparedness and Response Supplemental Appropriations Act, 2020” was created in an effort to encourage and promote the use of telemedicine services in replacement of traditional in-person care, slowing the growth of COVID-19 in our nation.
This bill made it simpler for providers to offer telehealth to Medicare beneficiaries while still receiving reimbursement for services. In the most recent developments of this legislation, CMS has expanded Medicare coverage to cover over 80 new telehealth services. Providers who offer these services to their eligible patients are able to bill at the same rate as in-person visits.
Expanded Telehealth Coverage From CMS
CMS is now reimbursing providers for more than 80 new telehealth services offered Medicare members. The new government plan has put temporary rulings in place, prompting CMS to pay for remote monitoring services for conditions related to the coronavirus as well as many unrelated to the virus, such as vital monitoring.
These additional services include emergency department visits, initial nursing facility related visits, and in-home visits provided by qualified clinicians that are offering telehealth.
According to a fact sheet shared by CMS, they are “allowing telehealth to fulfill many face-to-face visit requirements for clinicians to see their patients in in-patient rehabilitation facilities, hospice, and home health.” Throughout the duration of the pandemic, patients are able to use regularly available audio/visual communication apps to visit with their provider.
Increase Popular Use of Telehealth Among Senior Beneficiaries
Senior citizens are some of the most vulnerable during this season as the symptoms of the coronavirus can be much more severe for those over the age of 65. With 97% of seniors in the United States covered by Medicare, they have a lot to gain through these developments in telehealth coverage.
With accessible service options and fewer restrictions, it is expected that a growing number of seniors, covered under traditional Medicare, will utilize telehealth now and in the future. Those who have been hesitant to utilize remote care options up to this point will continue to use them once the coronavirus pandemic has ended.
Remote monitoring services can be life-changing for those suffering from chronic conditions, allowing them to stay home rather than travel to and from their physician’s office for testing and treatment. With the large majority of seniors in the United States battling at least one chronic condition, telehealth options can help them achieve a better quality of care and quality of life.
Telehealth offers a safe option for Medicare patients to continue receiving the care they need throughout the COVID-19 outbreak, keeping them in their homes and nursing facilities, and away from potential risks. To learn more about a quality solution that can help your organization offer telehealth services to your patients, click here.